AHEC Scholars Summer Projects and Public Health Projects


2025 AHEC Scholars Summer Projects
Larner College of Medicine students from the class of 2028 are invited to apply. The summer program is an 80-hour pathway activity that meets requirements for one year of AHEC Scholars activity.
Summer projects information session: Wednesday, January 22, 2005 noon-1:00 in Med Ed 200 Sullivan Classroom. Click here to view Session Slides. Questions about AHEC Scholars or the AHEC Scholars Summer Program can be directed to Patti S. Urie at patti.smith-urie@uvm.edu.
Application period is closed. Applicants will be notified in early March.
A common application is used to apply to summer projects hosted by three organizations: UVM AHEC, Northern VT AHEC, and Southern VT AHEC.
Projects are typically 100 hours (40 didactic hours and 60 field-based/project-specific hours) and pay a $1,500 stipend. This is a competitive process with limited enrollment capacity. Decisions are based on the best match for each program.
Summer projects fall into one of two tracks: Research and Quality Improvement or Mentoring and Education. All projects will link to one or more AHEC focus areas:
- Interprofessional Education/Interprofessional Practice
- Behavioral Health Integration
- Connecting Communities and Supporting Health Professionals (CHWs)
- Virtual Learning and Telehealth
- Social Determinants of Health
- Cultural Competency
- Medical Practice Transformation
- Current and Emerging Health Issues (Opioids and Substance Use Disorders, Oral Health as part of Overall Health, COVID-19)
2024 AHEC Scholars Summer Projects
Click to view: AHEC Scholars 2024 Summer Projects description
Track: Research/Quality Improvement (projects completed by teams of 2-5 students, UVM AHEC faculty, UVM Health Network faculty, and community partners)
Immigrant Health Insurance Plan (IHIP) Projects
Three summer projects teams worked with the Office of the Health Care Advocate (HCA) at Vermont Legal Aid on various aspects of IHIP rollout over the past two years. In 2022, the Vermont legislature enacted the Immigrant Health Insurance Plan (IHIP) to provide health insurance for pregnant people and children under the age of 19 who do not qualify for Medicaid due to immigration status. One team sought to asses whether current outreach and educational materials effectively prepare healthcare professionals, advocates, and community organizations to identify and enroll eligible individuals. A second team aimed to identify barriers and potential program improvements for enrollees and those eligible to enroll. A third team looked at potential expansion of health insurance programs to other groups of Vermonters who do not qualify due to immigration status.
 UVM ScholarWorks: "Vermont Immigrant Health Insurance Plan: Outreach and Education" by Eunice Suberu, Harsimran Multani et al.
UVM ScholarWorks: "Vermont Immigrant Health Insurance Plan: Outreach and Education" by Eunice Suberu, Harsimran Multani et al.
Eunice Suberu, Harsimran Multani, and Jake Reigle presented findings to DVHA stakeholders on September 5, 2024.
Eunice Suberu presented the poster at the SNMA RMEC conference in Boston, MA on October 5, 2024.
Eunice Suberu, Harsimran Multani, and Jake Reigle presented the poster at the Vermont Medical Society annual meeting on November 1, 2024 and were awarded second place.
Medical Education Project
Continuous-glucose monitoring (CGM) is a technology used by patients with diabetes to monitor and respond to blood-glucose levels (BGL). Despite proven benefit to patients, providers may not be comfortable prescribing or interpreting data from these devices. Teaching students about CGMs has the potential to increase not only their familiarity with this technology, but also complement their understanding of metabolism and nutrition concepts. This study examined the use of CGM as an educational tool in parallel with a traditional pre-clinical medical curriculum.

UVM ScholarWorks: "Continuous Glucose Monitoring in Medical Education: Bridging pre-clinical sciences with the patient experience" by Caitlin Beattie, Cassandra Chin et al.
Claudia Tarrant, Cassandra Chin, and Caitlin Beattie presented the poster on October 18th at the ACP 2024 Vermont Chapter Annual Scientific Meeting in Stowe, VT.
Electronic Medical Record Projects
The Electronic Medical Record (EMR), while an essential part of healthcare, can be complex and confusing. The informatics team, which includes physician-informaticists, is continuously engaged in projects to improve daily workflows for safety and efficiency. AHEC Scholars students have completed many successful EMR Projects, including patient portal messaging, standardization of documentation, and patient centered care. 2024 Projects include:
 UVM ScholarWorks: "The Impact of Epic Secure Chat on Clinicians and Patient Care" by Jai Narain, Rachel McEntee, MD et al.
UVM ScholarWorks: "The Impact of Epic Secure Chat on Clinicians and Patient Care" by Jai Narain, Rachel McEntee, MD et al.
Poster presented by Jai Narain at The North American Primary Care Research Group (NAPCRG) annual meeting on November 20, 2024 in Quebec City, Canada.
 UVM ScholarWorks: "Patient Perception of Artificial Intelligence Generated Note Quality" by Francisco Cordero, Varsha Pudi et al.
UVM ScholarWorks: "Patient Perception of Artificial Intelligence Generated Note Quality" by Francisco Cordero, Varsha Pudi et al.
Poster presented by Francisco Cordero at The North American Primary Care Research Group (NAPCRG) annual meeting on November 20, 2024 in Quebec City, Canada.
 UVM ScholarWorks: "Evaluating Patient Portals for Patients with Visual or Hearing Impairments: Provider Confidence and Communication Challenges" by Jonathan Chen, Garrett Wu et al.
UVM ScholarWorks: "Evaluating Patient Portals for Patients with Visual or Hearing Impairments: Provider Confidence and Communication Challenges" by Jonathan Chen, Garrett Wu et al.
Poster presented by Francisco Cordero at The North American Primary Care Research Group (NAPCRG) annual meeting on November 20, 2024 in Quebec City, Canada.
 UVM ScholarWorks: "Comparison of Provider-Generated vs Artificial Intelligence-Generated Medical Encounter Notes" by Edward Harrington, Francisco Cordero et al.
UVM ScholarWorks: "Comparison of Provider-Generated vs Artificial Intelligence-Generated Medical Encounter Notes" by Edward Harrington, Francisco Cordero et al.
Poster presented by Edward Harrington at The North American Primary Care Research Group (NAPCRG) annual meting on November 20, 2024 in Quebec City, Canada.
 UVM ScholarWorks: "Investigating Disparities in EHR Workload: Increased Burden of Patient Advice Request Messages on Female Physicians" by Lauren Schiff, Julianne Scholes et al.
UVM ScholarWorks: "Investigating Disparities in EHR Workload: Increased Burden of Patient Advice Request Messages on Female Physicians" by Lauren Schiff, Julianne Scholes et al.
Poster presented by Lauren Schiff at The North American Primary Care Research Group (NAPCRG) annual meeting on November 20, 2024 in Quebec City, Canada.
 UVM ScholarWorks: "Developing a Comprehensive Barrett's Esophagus Pathway with Clinical Support Tools" by Evan Baugh, Eric Ganguly et al.
UVM ScholarWorks: "Developing a Comprehensive Barrett's Esophagus Pathway with Clinical Support Tools" by Evan Baugh, Eric Ganguly et al.
 UVM ScholarWorks: "Enhancing Provider Confidence in Communicating with Patients with Limited English Proficiency (LEP) Through Patient Letters" by Garrett Wu, Jonathan Chen et al.
UVM ScholarWorks: "Enhancing Provider Confidence in Communicating with Patients with Limited English Proficiency (LEP) Through Patient Letters" by Garrett Wu, Jonathan Chen et al.
Poster presented by Garrett Wu at The North American Primary Care Research Group (NAPCRG) annual meeting on November 20, 2024 in Quebec City, Canada.
Food Systems Project
Access to healthy food is a critical social determinant of health. LCOM students worked with partners from Champlain Valley Office of Economic Opportunity (CVOEO) food shelf programs to create an electronic survey embedded in the ordering software families use to access food. The survey aimed to better understand the opinions, usage, and challenges of English vs. non-English speakers who utilize the program.
 UVM ScholarWorks: "Opinions and Utilization of Burlington Mobile Food Pantry by English and non-English Speaking Individuals" by Isabel Thomas, Kristin Reed et al.
UVM ScholarWorks: "Opinions and Utilization of Burlington Mobile Food Pantry by English and non-English Speaking Individuals" by Isabel Thomas, Kristin Reed et al.
LGBTQ Health Project
Dental healthcare is important for preventative care and overall health. Compared to other types of medical trainees, dental students and residents have less formal training in providing inclusive care for LGBTQIA+ patients. Many queer-identifying patients have significant barriers to dental care, a significant one being providers' lack of understanding of queer identities and best practices for treating queer and transgender patients. This project aimed to learn more about the knowledge gap related to LGBTQIA+ dental care and interest in educational opportunities among Vermont dental professionals.

UVM ScholarWorks: "Development of an LGBTQIA+ Video Curriculum for Vermont Dental Offices" by Marina Cannon, Elliot Culleen et al.
 Marina Cannon, Ell Culleen, and Amir Zafaranian presented the poster at the 2024 UVM Health Equity Summit -- Building Solidarity: Sustainable Pathways towards Health Equity -- on October 7, 2024
Marina Cannon, Ell Culleen, and Amir Zafaranian presented the poster at the 2024 UVM Health Equity Summit -- Building Solidarity: Sustainable Pathways towards Health Equity -- on October 7, 2024
Track: Education/Mentoring (Northern Vermont AHEC and Southern Vermont AHEC)
The Governor's Institutes of Vermont
Institute on Health & Medicine
The Governor's Institute on Health and Medicine is a week-long, health science enrichment and career exploration camp for high school students. LCOM students serve as residential mentors to support students' learning and assist in creating a fun and respectful learning community. Content is delivered through hands-on activities, scenario-based learning, and case discussion. Health & Medicine North/South Institute 2024 Recap Video.
Click below for photo album highlights:




2023 AHEC Scholars Summer Projects
Click to view: AHEC Scholars 2023 Summer Projects program description
Track:
Research/Quality Improvement (projects completed by teams of 2-5 students, UVM
AHEC faculty, UVM Health Network faculty, and community partners)
Food Systems Project
Access to healthy food is a critical social determinant of health. LCOM students worked with partners from Champlain Valley Office of Economic Opportunity (CVOEO) food shelf programs to score the nutritional value of foods stocked and distributed in two Vermont counties. A data presentation for food shelf representatives can be viewed in UVM ScholarWorks.
UVM ScholarWorks: Nutritional Evaluation of Food Bank Services in Chittenden and Addison Counties, Vermont
Electronic Medical Record Projects
The Electronic Medical Record (EMR), while an essential part of healthcare, can be complex and confusing. The informatics team, which includes physician-informatacists, is continuously engaged in projects to improve daily workflows for safety and efficiency. AHEC Scholars students have completed many successful EMR Projects, including patient portal messaging, standardization of documentation, and patient centered care. 2023 Projects include:

UVM ScholarWorks: Provider Perspectives on Language Barriers in MyChart Enrollment for Patients with Limited English Proficiency
Poster presented by Shruthi Santhanakrishnan and Kassandra Mastras, LCOM class of 2026, at ACP Vermont Chapter Annual Scientific Meeting on Friday, September 29, 2023. The poster won in the medical student research category and will be presented at the national ACP conference in April, 2024. Congratulations, Shruthi and Kassie!
/ahec-images/mychart_provider_poster_16_9_(002).tmb-medium.jpg?sfvrsn=329a0d90_1) UVM ScholarWorks: Primary Care Provider MyChart Patient Advice Request Message Gender-Specific Workload at University of Vermont Health Network
UVM ScholarWorks: Primary Care Provider MyChart Patient Advice Request Message Gender-Specific Workload at University of Vermont Health Network
Poster presented by Kristen Karpowicz and Julie Scholes, LCOM class of 2026, at ACP Vermont Chapter Annual Scientific Meeting on Friday, September 29, 2023.

UVM Scholarworks: MyChart Messaging: Patient Preferences about Timing of Provider Responses to Medical Advice Requests
Poster presented by Kristen Karpowicz and Julie Scholes, LCOM class of 2026, at ACP Vermont Chapter Annual Scientific Meeting on Friday, September 29, 2023.
 UVM ScholarWorks: Primary Care Provider Perspectives on APSO Note Templates at UVM Health Network
UVM ScholarWorks: Primary Care Provider Perspectives on APSO Note Templates at UVM Health Network
Poster presented by Anna Landis and Hayden Christensen, LCOM class of 2026, at ACP Vermont Chapter Annual Scientific Meeting on Friday, September 29, 2023.
Communication Disabilities in Healthcare
Patient-provider communication is a foundational element of healthcare delivery, but may be influenced by communication disabilities. Approaches to improve clinical communication include bringing a “communication companion” along to visits, use of a written after-visit summary, communication via an electronic patient portal, and others. This study sought to determine patient preferences regarding the roles of a communication companion and other approaches to overcoming communication challenges.
 UVM ScholarWorks: Assessing Patient Preferences for Communication Companions in Primary Care
UVM ScholarWorks: Assessing Patient Preferences for Communication Companions in Primary Care
Anika Advant and Georgia Babb, LCOM class of 2026, presented project findings at the Third Annual Disability Advocacy Coalition in Medicine Interprofessional Virtual Conference: Intersectionality in Disability Medicine conference on October 28, 2023.
Vermont Office of the Healthcare Advocate - Medical Debt Project
According to a 2021 Vermont Department of Health survey, 35% of uninsured patients and 17% of insured patients reported owing medical debt in Vermont. In Vermont, Medicaid provides near universal coverage health insurance for low-income individuals. In contrast, Medicare has gaps that can leave beneficiaries with substantial out-of-pocket costs, especially for those who do not qualify for Medicare Savings Programs (MSPs). This project sought to understand healthcare affordability for Vermonters transitioning to Medicare by gaining perspectives from patients and healthcare stakeholders.
/ahec-images/ahec_poster_vms_16_9_(002).tmb-medium.jpg?sfvrsn=b0a3c47f_1)
UVM ScholarWorks: Understanding Affordability of Healthcare in Vermont
Jackson Bressor, Elle Cunningham, Khadija Moussadek, Lauren Tien, and Sarah Yang, LCOM class of 2026 presented project findings at the Vermont Medical Society Annual Meeting
Health Equity and Patient Centered Care in the Medical Home: Review and Update to Wellness and Screening Forms
Primary care settings are working on changes to be more inclusive and affirming to patients at risk for health disparities (LGBTQ, racial, ethnic, and socioeconomic groups). Signage and communication in the patient visit can enhance or hinder quality of care. Forms and screening tools can both create an inclusive welcoming environment or further alienate populations. The aim of this study was to enhance patient-provider communication through incorporation of patient-centered language on intake forms through The University of Vermont Medical Center (UVMMC).
 UVM ScholarWorks: Enhancing Health Equity Through Patient-Centered Care:Updating Screening Forms in a Primary Care Setting
UVM ScholarWorks: Enhancing Health Equity Through Patient-Centered Care:Updating Screening Forms in a Primary Care Setting
AHEC Interprofessional Challenge Project: Prevention of Firearm Injury
Each year in Vermont, approximately 75 people die from gunshot wounds and 65 are injured. The majority of these deaths are suicides, while the majority of injuries are caused by unintentional discharge. This project team consisted of two Larner Medical Students, one Public Health student and one Clinical Mental Health student. The team surveyed health care providers to assess current practices in firearm safety discussions with patients and the need for patient information materials.
UVM ScholarWorks: Firearm Safety Education in Vermont
Primary
Care Provider Opinions on Psychedelic Therapy
Psychedelics, such as MDMA, LSD, psilocybin, and ketamine, are mind-manifesting substances that have gained interest among academic, research, and policy stakeholders due to their potential as therapeutic agents for intractable mental health disorders. This project sought to understand Vermont providers’ knowledge and attitudes.
 UVM ScholarWorks: Vermont Primary Care Provider Knowledge and Attitudes Regarding Psychedelics
UVM ScholarWorks: Vermont Primary Care Provider Knowledge and Attitudes Regarding Psychedelics
Mallory Stultz and Cole Zweber, LCOM Class of 2026, presented at the Northeast Regional Society of General Internal Medicine Conference in Boston, MA on November 4, 2023.
Track: Education/Mentoring (Northern Vermont AHEC and Southern Vermont AHEC)
The Governor's Institute on Health and Medicine
July 9-15, 2023 Northern Vermont University Lyndon CampusThe Governor's Institute on Health and Medicine is a
week-long, health science enrichment and career exploration camp for high
school students. LCOM students serve as residential mentors to support
students’ learning and assist in creating a fun and respectful learning
community. Content is delivered through hands-on activities, scenario-based
learning, and case discussion.
MedQuest MentorsJuly 24-26, 2023 at Springfield Hospital and
North Star Health and August 2-4, 2023 at Rutland Regional Medical Center
MedQuest 2023 is an on-site, 3-day, non-residential
program for high school students to explore a variety of health careers in a
rich learning environment with engaging content and group discussions,
skill-building activities, job shadowing, mentoring, and dialogue with health
professionals. LCOM student mentors assist in preparing and presenting
materials to students and facilitate small group discussions and activities.
Advanced MedQuest Mentors
June 26-June 30, 2023 at Rutland Regional Medical Center
and Vermont State University at Castleton
Advanced MedQuest is an on-site, 5-day, non-residential
program for high school students who have previously completed MedQuest.
Students participate in an intensive job shadow experience and learn via
hands-on experience.
Pre-medical/Pre-health Enrichment Program for VTSU (PEP)
Two LCOM students teamed with SVT AHEC to work on PEP-VTSU an extracurricular enrichment program being developed for Vermont State University students interested in health professions. The program is geared toward professions in high demand in Vermont, with emphasis on meeting the needs of the Vermont health care workforce.
2021-2022 AHEC Scholar Summer Projects
Electronic Medical Record Project
UVM ScholarWorks: 21st Century Cures Act: Patient Perceptions on Open Information Sharing in Vermont Primary Care Clinics


Poster presentation at the April 2023 American College of Physicians (ACP) conference in San Diego, CA, by Jared Stone and Anthony Quach.
2022 Ethical Dilemmas in Medicine: Medical Repatriation
UVM ScholarWorks: Medical Repatriation in Vermont: The Current Landscape and Recommendations

Eating Disorders Project
Project Poster: Assessing the Current State of Eating Disorder Medical Education at LCOM

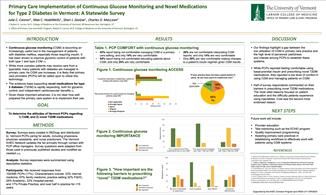
2021 AHEC Scholars Summer Project: Primary Care Implementation of Continuous Glucose Monitoring and Novel Medications for Type 2 Diabetes in Vermont: A Statewide Survey
Audio presentation
Poster
Public Health Projects with Medical Students
Public Health Projects (PHP), a required course incorporated in the Vermont Integrated Curriculum, teaches second-year medical students to apply the principles and science of public health while working to improve the health of the community.
Public Health Projects respond to health needs identified by local community agencies. 16 projects are completed each fall by medical student groups working in partnership with community agencies, and mentored by both College of Medicine faculty
and community agency mentors.
FY21
Project: "Naturopathic
Medicine in Vermont's Healthcare System: A Thematic Analysis"
Abstract: Background:--Naturopathy
is a practice of medicine that emphasizes natural therapies. In Vermont,
Naturopathic doctors (NDs) are eligible for full prescriptive authority and may
be designated as primary care providers, however their specific role within the
healthcare system is not well understood. The objective of this project was to explore
the role of NDs in Vermont’s healthcare system.
Medical Students (class of 2024): Trevor Coles, Tayler Drake, Rosie Eiduson, Dan Fried, Max HoddWells, Simran Kalsi, Mahima Poreddy
UVM Faculty Mentor: Charles MacLean, MD
Community Agency Mentor: Elizabeth Cote
Naturopathic Medicine in Vermont's Healthcare System: A Thematic Analysis Abstract
Naturopathic Medicine in Vermont's Healthcare System: A Thematic Analysis Poster
FY19
Project: "Opinion and Attitudes of Vermont School Principals and Nurses on Youth Vaping"
Abstract: Background--A rapidly emerging new trend that is turning into a nationwide epidemic for youth in the United States is the use of electronic vapor products also known as “e-cigs”, “e-hookahs”, “vapes”,
“mods”, and “JUULS”. There is little known about the long-term health effects of prolonged use of vapes. The rise in vape products sales and use, poses a public health threat to adolescents. The study’s purpose is
to assess the opinions and attitudes of school principals and nurses about youth vaping. The results will identify if any gaps exist in the youth vaping issue and further expand on existing concerns of school issues. Using this information, public
health recommendations can be developed.
Student: Vy Cao, MPH (UVM Class of 2019)
UVM Faculty Mentors: Charles MacLean, MD and Katherine Mariani, MD
Community Agency Mentor: Elizabeth Cote
Youth Vaping Abstract
Youth Vaping Poster
Project: "Vermont Legislators' Opinions Regarding the Opioid Epidemic"
 One of the Public Health projects presented by the students in the Larner College of Medicine Class of 2021, "Vermont Legislators' Opinions Regarding the Opioid Epidemic" was performed in partnership with the UVM AHEC Program.
One of the Public Health projects presented by the students in the Larner College of Medicine Class of 2021, "Vermont Legislators' Opinions Regarding the Opioid Epidemic" was performed in partnership with the UVM AHEC Program.
Abstract: Background--In response to the opioid crisis, the 2018 Vermont legislative session proposed 22 bills, nine of which passed. While there is literature that includes various legislators' information source preferences,
there is no literature regarding how Vermont State Legislators gather information and formulate public health decisions surrounding opioid policies. The goals of the study were 1) to identify Vermont legislators' opinions regarding investments
in, and effects of, programs to prevent and treat opioid addiction, and 2) to determine sources of information used and valued by legislators.
Pictured from left: Ryan Harned, Bridget Moore, Casandra Nowicki, Matthew Lebrow, Emily Eichner, Jonathan Gau, and Liam du Preez
Medical Students (class of 2021): Casandra Nowicki, Emily Eichner, Liam du Preez, Jonathan Gau, Matthew Lebow, Bridget Moore, Ryan Harned
UVM Faculty Mentors: Charles D. MacLean, MD and Jan K. Carney MD, MPH
Community Agency Mentor: Elizabeth Cote
Vermont Legislators' Opinions Regarding the Opioid Epidemic Abstract
Vermont Legislators' Opinions Regarding the Opioid Epidemic Poster
FY18
 One of the Public Health projects presented by the students in the Larner College of Medicine Class of 2020, "Prescriber Perspectives of July 1, 2017 Opioid Prescribing Rules" was performed in partnership with the UVM AHEC Program.
One of the Public Health projects presented by the students in the Larner College of Medicine Class of 2020, "Prescriber Perspectives of July 1, 2017 Opioid Prescribing Rules" was performed in partnership with the UVM AHEC Program.
Abstract: Introduction--In July 2017, Vermont enacted new rules on acute opioid prescribing to reduce misuse, addiction, and overdose associated with prescription opioids. The new rules include requirements of non-opioid therapy
use when possible, querying VPMS, patient education and informed consent, and co-prescription of naloxone. Our study objective was to gain insight into the perspectives of opioid prescribers on the new rules read more.
Medical Students (class of 2020): Zara S. Bowden, Jinal Gandhi, S. Natasha Jost, Hanna Mathers, Chad Serels, Daniel Wigmore, and Timothy Wong
Pictured from left: Timothy Wong, Chad Serels, S. Natasha Jost,
Jinal Gandhi, Hannah Mathers, Zara S. Bowden, and Charles MacLean, MD (missing from photo: Daniel Wigmore)
UVM Faculty Mentors: Charles D. MacLean, MD and Jan K. Carney MD, MPH
Community Faculty: Elizabeth Cote
Prescriber Perspectives of July 1, 2017 Opioid Prescribing Rules Abstract
The 2017 Vermont Opioid Prescribing Rules: Prescriber Attitudes Poster
FY17
 Students in the Larner College of Medicine Class of 2019 presented posters and explained findings from 16 different Public Health projects at a public reception and
celebration on January 18, 2017.
Students in the Larner College of Medicine Class of 2019 presented posters and explained findings from 16 different Public Health projects at a public reception and
celebration on January 18, 2017.
One of the 16 student projects, “Patient Perspectives on Medication Assisted Therapy in Vermont” was performed in partnership with the UVM AHEC Program.
Vermont has the highest per capita buprenorphine use in the U.S. The UVM AHEC Program's PHP cohort aimed to gain a better understanding of patient perspectives on the barriers and enablers of successful Medication-Assisted Therapy (MAT) – buprenorphine
treatment for opioid addiction – in order to help inform system refinement. The students developed an interview guide based on established tools, as well as input from program leaders, clinicians and community stakeholders, and conducted
interviews with 44 patients at two specialty treatment centers in Burlington, VT in October 2016. The students found that half of the subjects reported a mental health condition and stated that barriers to treatment included transportation (25
percent) and stigma (41 percent), among other factors. The students advised that “a comprehensive system that addresses this wide range of domains is critical to achieving optimal outcomes."
Medical Students (class of 2019): Ashley Adkins, Holly Bachilas, Florence DiBiase, Michael Marallo, John Paul Nsubuga, Lloyd Patashnick, Curran Uppaluri
Pictured (from left): Holly Bachilas, Florence DiBiase,
John Paul Nsubuga, Curan Uppaluri, and Michael Marallo
UVM Faculty Mentor: Charles MacLean, MD and Jan Carney, MD, MPH
Community Faculty: Elizabeth Cote
MAT Patient Perspectives Poster
Patient Perspectives on MAT Abstract
FY16
Students in the Larner College of Medicine Class of 2018 presented posters and explained findings from 16 different Public Health projects at a public reception and celebration on January 20, 2016. One project, “Addressing the Opioid Crisis
in Vermont: Lessons Learned from Primary Care Physicians,” was sponsored by the UVM Office of Primary Care and statewide Area Health Education Centers (AHEC) Program. The goal of the project was to identify physician barriers to providing
office-based opioid treatment (OBOT) in Chittenden County. The students who conducted the study are Timothy Henderson, Molly Markowitz, Adam Petchers, Brittany Rocque, Andrew Sheridan, Nathaniel Sugiyama, and Lindsey Wyatt. Their UVM faculty mentors
are Charles MacLean, MD, and Jan Carney, MD, MPH; community faculty members are Beth Tanzmen, MSW, Assistant Director, Vermont Blueprint for Health, and Elizabeth Cote, director, Office of Primary Care and AHEC.
Of the 25 primary care physicians interviewed, non-office-based opioid treatment providers more frequently reported that OBOT patients were challenging. OBOT providers more frequently acknowledged the stigma associated with OBOT. Both groups of physicians
expressed a desire for increased state support for OBOT. The student recommendations are: increased state support/resources for OBOT; mentorship of new OBOT providers by experienced OBOT providers; and generation of OBOT best practice guidelines
for primary care providers.
Asked what they were most surprised by in their study, Lindsey Wyatt said it was the fact that almost every provider said OBOT was easier and more rewarding than they thought it would be.
The Class of 2018 medical students working on this project found that "the five most frequently reported barriers were: insufficient state logistical support, challenging patient population, practice infrastructure/capacity, time, and provider fears/concerns.
Seventy-nine percent of non-prescriber PCPs said that they would provide OBOT if the identified barriers were removed."
“Addressing the Opioid Crisis in Vermont: Lessons Learned from Primary Care Physicians.” (PDF)
An Inter-Professional Exploration of Cuba’s Primary Healthcare System
This presentation gives an overview of learning from a June 2014 trip to Cuba by faculty in the Larner Colleges of Medicine, Social Work, and College of Nursing and Health Sciences; medical students, a dental student, a dental technician, a social
work graduate student, a nurse practitioner student; and members of the Burlington College faculty. The purpose of the course was to gain a better understanding of the Cuban health system, particularly the role of primary care, and the interaction
between primary care, public health and the community. Cuba has a well-regarded system of population health and primary care.
Exploring Cuba's Primary Healthcare System (PDF)