Traveling roughly 90 miles to the White River Junction, Vt.-based Veterans’ Administration Medical Center from the Burlington, Vt. area can be difficult, especially in winter. It’s even more challenging for the veteran who is living with chronic pain or has been diagnosed with a sleep disorder or cardiac arrhythmia.
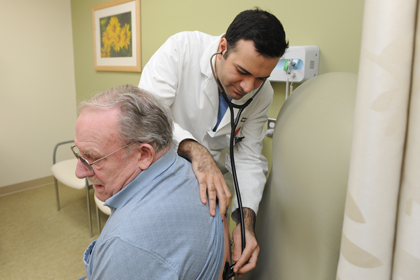
Cardiology fellow Amir Azarbal, M.D., examines a patient at the V.A. Lakeside Clinic in Burlington (Photo: David Seaver)
Traveling roughly 90 miles to the White River Junction, Vt.-based Veterans’ Administration Medical Center from the Burlington, Vt. area can be difficult, especially in winter. It’s even more challenging for the veteran who is living with chronic pain or has been diagnosed with a sleep disorder or cardiac arrhythmia. And if he or she doesn’t drive or have access to a car, it’s virtually impossible.
These Vermont variables – weather and geography – make access to V.A. health services in Burlington that much more important. Although the V.A. has had a presence in Burlington for many years, the October 2013 opening of a new location, called the Lakeside Clinic, combined with an ongoing partnership with the University of Vermont Department of Medicine, continues to expand care options for local veterans. Fourteen internal medicine residents routinely spend some 20 days of their outpatient medicine experience at the clinic, seeing patients who struggle with comorbid issues at a rate greater than the general population.
“It’s great for our residents to see how care, as we move forward, is going to look in the outpatient setting,” says Mark Pasanen, M.D., associate professor of medicine in the division of hospitalist medicine and director of the Internal Medicine Residency Program. The time at Lakeside, he adds, offers them “added exposure to an advanced, patient-centered medical home model.”
“It’s a good experience for them to see patients with multiple chronic diseases and comorbidities in that setting, because not everyone needs to be in an emergency room – they can be seen in an acute clinic setting and be well taken care of,” says Mark Levine, M.D., associate dean for graduate medical education.
And residents, fellows, and faculty are providing specialized care that might otherwise have slipped through the cracks. Since a dermatology clinic was launched at Lakeside in October 2015, for example, more than 50 skin cancers have been biopsied, says Joseph Pierson, M.D., assistant professor of medicine in the division of dermatology and director of the Dermatology Residency Program.
“It has been a challenge to get them to worry about sun exposure,” says Pierson of members of the military. “They’re more worried about their Kevlar equipment being worn properly.”
Veterans who are diagnosed with skin cancer have the option of being treated in White River Junction or at UVM Medical Center. For those who need more delicate Mohs surgery, the nearest V.A. location is Boston; however, the UVM partnership offers a much closer alternative. It’s also allowed dermatology to add a seventh resident at the White River Junction V.A., which has historically been affiliated with Dartmouth-Hitchcock Medical Center. This new relationship marks the first time the V.A. has entered into a joint venture in graduate medical education with the UVM Medical Center.
“It’s a nice way to have the two institutions – UVM and Dartmouth – collaborate around the care of the northern New England veteran population in a patient-centered manner,” says Levine.
Cardiology’s relationship with the V.A. goes back more than a decade. It’s an obvious fit; with a population that skews toward older males, there is plenty of cardiovascular disease, says David Schneider, M.D., professor of medicine and director of the division of cardiology.
“From our perspective, there was a clinical need there that dovetailed nicely with an educational opportunity,” he says, echoing others in calling the V.A. partnership a “win-win.” Fellows take a fully active role in patient care, serving as primary caregivers and reviewing findings and treatment plans with attending physicians. “So the patients are getting the best care, but the fellow is really driving the interaction with the patient, which gives them that level of responsibility and provides a great learning environment,” says Schneider.
Spending time at the Lakeside Clinic means that in addition to focusing on their specialties, all residents and fellows face a fairly unique set of issues, including military-related injuries, chronic pain, prosthetics, and post-traumatic stress disorder, says Jonathan Cohen, M.D., M.P.H., director of the clinic. They’re also exposed to integrated care in action, with physical therapy, cognitive psychotherapy, audiometry, acupuncture, and yoga onsite. Telehealth is routinely used as well. But the benefits are mutual.
“It’s great for the V.A., Cohen says. “Not only does it take some of the pressure off the White River Junction–based providers, we like having them in the clinic because it’s nice to collaborate with subspecialists.” Cohen adds that there are possibilities for continued program growth, made possible in part by the 2014 Veterans Health Care Bill.
The newest focus at Lakeside is sleep medicine. Susan Dunning, M.D., assistant professor of medicine in the division of pulmonary disease and critical care medicine and director of the UVM Medical Center Sleep Program, established a limited sleep clinic there in late December 2015, but she expects it to reach capacity quickly and hopes to expand it as needed. For now, Dunning and one sleep fellow see V.A. patients who are referred for sleep problems, particularly sleep-related breathing disorders, along with other disorders such as insomnia, hypersomnias, parasomnias and sleep movement disorders. They also optimize treatment with respiratory-assist devices (CPAP or BiPAP) for sleep-related breathing disorders. Dunning is planning to start a mask-fit clinic, and anticipates that Lakeside will eventually function as a community-based durable medical equipment supplier of respiratory-assist equipment for V.A. patients in the Burlington area. In addition, sleep medicine patients will be able to undergo polysomnogram studies at UVM Medical Center; the nearest V.A. facilities that provide this service are in Boston and Albany.
“The Lakeside clinic provides a great opportunity to have veterans’ medical needs met closer to home,” says Dunning.
As these clinical partnerships continue to thrive, the Department of Medicine is now also exploring the possibility for research collaborations.