/com-top-tier-images/deansnewsletter/recurring_graphics/dean_newsletterheader_600px_blue(2).jpg?sfvrsn=3b747039_2)
February 24, 2021 | Volume III, Issue 4
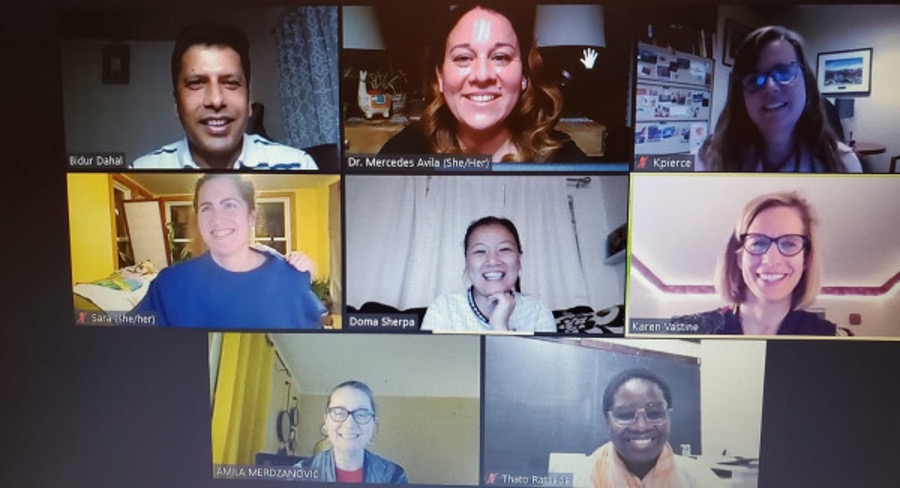
A Matter of Trust: Bringing Vaccine Education to New American Communities
One of the most alarming realizations of the past year has been the clear link between structural racism in the U.S. and the racial and ethnic health disparities that have led to a disproportionate impact of COVID-19 on communities of color. According to the Centers for Disease Control and Prevention, compared to white, non-Hispanic persons, COVID-19 infection, hospitalization, and death rates are three to four times higher in BIPOC (Black, Indigenous, People of Color) communities.
It’s a grave statistic — and one that is alarming for Vermont’s New American community and those who work with them.
Over the last two decades, members of the VT LEND program, including its director, Maria Mercedes Avila, Ph.D., have built connections with the New American community as they research health disparities within Vermont and work to build community trust.
Trust is a critical factor when it comes to administration of COVID-19 vaccines. Focus groups conducted with Black, Indigenous, Hispanic/Latinx, immigrant and refugee community leaders, including Dr. Avila, serving on Vermont’s Health Disparities and Cultural Competence Committee, revealed that New American community members had a general sense of distrust, based on the long history of unethical medical research involving underserved communities across the globe, and concerns about the vaccine. Those findings encouraged Dr. Avila and partners, including Karen Vastine, a senior officer in the UVM Health Network’s community relations office, Amila Merdzanovic of the U.S. Committee for Refugees and Immigrants-Vermont (USCRI-VT), and Thato Ratsebe of the Association of Africans Living in Vermont (AALV-VT), to take a proactive educational approach to ensure vaccine adherence in the communities that needed it most.
The partners quickly pulled together necessary elements for education sessions featuring Kristen Pierce, M.D.,professor of medicine, infectious disease specialist, and vaccine expert. In collaboration with community leaders, they scheduled virtual education sessions, hired interpreters and cultural liaisons, and rolled out the first four evening educational sessions in December.
The format and goal of the sessions are simple: share the reasons why it’s important to get the vaccine and answer questions to encourage community members to get the vaccine. By the end of this month, they will have held another nine sessions – each in a different language – and have four more scheduled in March.
Read the full article about the Community Education Sessions on the COVID-19 Vaccine.
Pictured above: Partners in the Community Education Sessions on the COVID-19 Vaccine gather following a Zoom session, including (top row, left to right) Bidur Dahal, VT LEND education coach outreach professional and Nepali community cultural broker; Dr. Avila; Dr. Pierce; (middle row, left to right) Sara Chesbrough, Vermont Department of Health; Doma Sherpa, AALV-VT and a cultural broker; Ms. Vastine; (bottom row, left to right) Ms. Merdzanovic; and Ms. Ratsebe.

LHOMe Initiative Fills Crucial Gap for Medical Students
During their education, medical students learn about social determinants of health and how these factors will inform care plans for future patients. At the same time, many of these students are experiencing these challenges first-hand, often without easy access to or knowledge of school-based or local support networks and resources.
The consequences of social determinants of health, such as food insecurity, unstable housing, and financial instability, disproportionately effect non-traditional students and students who are underrepresented in medicine. Often far from home and personal support networks, these students sometimes struggle to maintain their grades and balance curricular commitments, suffer mental health crises, and in some cases, must put their medical education on pause or leave school entirely.
Class of 2023 medical student Dana Allison and her team at the newly founded LHOMe Initiative are tackling this national issue head-on within the College. Through LHOMe, Ms. Allison and her colleagues seek “to help medical students meet all academic and professional expectations; improve academic performance; contribute to ongoing class-wide student support; and limit medical student attrition.”
“Dana’s LHOMe project has been absolutely crucial — filling an important gap in our understanding of medical students’ needs at a critical moment,” says Interim Associate Dean for Students and LHOMe faculty advisor Lee Rosen, Ph.D. “Dana and her collaborators led the way to helping us develop a language and a dialogue about issues related to basic needs and equity. These issues can be hard to discuss, but they only worsen in silence.”
Pictured above: Dana Allison, Class of 2023 medical student

Mind Body Buddy: Pediatrics Faculty Work to Treat the Whole Child
The number of children presenting with mental health issues is on the rise and pediatricians are often the first to assess how best to offer support. But finding help can be challenging – the number of mental and behavioral health specialists hasn’t kept pace with need, and during the pandemic, experts are seeing that gap widen even further.
Spurred by his own experience with anxiety as a teen and struggling with how to best support his patients’ mental health needs, Class of 2017 alum and Chief Pediatrics Resident Nick Bonenfant, M.D., set out to educate himself and, with collaborators in pediatrics and psychiatry, founded a four-week elective psychiatry rotation for second- and third-year pediatric residents and the “Mind Body Buddy” program. The elective was co-developed with Maya Strange, M.D., assistant professor and director of the Child Psychiatry Fellowship Program, and Elizabeth Forbes, M.D.,assistant professor of pediatrics and division chief of the UVM Children’s Hospital Children’s Specialty Center. Mind Body Buddy is a collaboration between the Departments of Pediatrics and Psychiatry that offers pediatric residents and child and adolescent psychiatry fellows real-time peer-to-peer support, cross-specialty lectures, and opportunities to attend patient appointments together.
In addition to Drs. Bonenfant, Strange, and Forbes, Mind Body Buddy collaborators included 2019-2020 Pediatric Chief Resident Anna Zuckerman, M.D.; Associate Professor and Director of the Pediatric Residency Program Jill Rinehart, M.D.; Assistant Professor of Psychiatry Haley McGowan, D.O.; Clinical Professor of Pediatrics Marshall “Buzz” Land, M.D.; Clinical Assistant Professor of Psychiatry Logan Hegg, M.D.; and Aamani Chava, M.D., clinical instructor of psychiatry and child and adolescent psychiatry fellow.
“The program brings us back to the basics and teaches us how to communicate effectively as specialists in our respective fields,” says Dr. Chava.
Pictured above: Drs. Bonenfant (left) and Chava.


 Schools must create a culture that normalizes the need for self-care and includes vulnerability as part of professionalism.”
Schools must create a culture that normalizes the need for self-care and includes vulnerability as part of professionalism.”
– From Class of 2021 medical student Chris Veal,
“We Burn Out, We Break, We Die: Medical Schools Must Change Their Culture to Preserve Medical Student Mental Health,” published in Academic Medicine.
Read more about Mr. Veal’s Commentary and Dean Page’s message to the Larner community.
Pictured at left: Chris Veal '21

Join the Celebration of Gender Equity in Medicine and Science online on Thursday, March 4, at 5:00 p.m.
(Zoom link will be emailed the week of March 1.)
Accolades & Appointments

Lee-Anna K. Burgess, M.D., has been appointed director of the Nutrition, Metabolism, Gastrointestinal System (NMGI) course in the Foundations Level of the Vermont Integrated Curriculum. Dr. Burgess has been a faculty member since 2018 and is an assistant professor of medicine in the Division of Hospital Medicine. She received her medical degree from the University of Queensland in Brisbane, Australia, and completed an internal medicine residency at UVM Medical Center, where she was Chief Resident from 2017–2018. She is the recipient of the 2017 Frank L. Babbott Memorial Resident of the Year Award and the 2020 Mark A. Levine Clinical Teacher of the Year Award. Her primary clinical interests are hospital medicine, high value care, and communication.

The New Hampshire Union Leader selected Larner College of Medicine Class of 2007 alum Benjamin Chan, M.D., as the 2020 NH Citizen of the Year. Dr. Chan, who has served as New Hampshire’s state epidemiologist since 2014, was recognized for his role as “the calm voice of science and reason that New Hampshire leaders and residents have turned to for facts, context and reassurance amid the fear and uncertainty of an unparalleled health and economic crisis.” Dr. Chan completed an internal medicine residency at Dartmouth-Hitchcock Medical Center and is board-certified in internal medicine, public health and preventive medicine, and infectious disease. Read the full article in the Union Leader here.

Debora Kamin Mukaz, Ph.D., postdoctoral associate in the Division of Hematology/Oncology in the Department of Medicine, was named to Cell Mentor’s 1,000 Inspiring Black Scientists, a recognition of “individuals who’ve helped push us to the next level.” Read more about this initiative on the Cell Mentor site.

Patrick Mullen, a doctoral student in the Neuroscience Graduate Program, is the recipient of the 2020-2021 Rodney L. Parsons Anatomy and Neurobiology Award, which honors Rodney Parsons, Ph.D., professor emeritus and former chair of anatomy and neurobiology. The award aims “to support outstanding graduate students who demonstrate excellence in both neuroscience research and teaching in any broadly defined anatomical science.” Mullen is mentored by Christopher Francklyn, Ph.D., professor of biochemistry, and Alicia Ebert, Ph.D., associate professor of biology.

J. Steele Taylor, M.D., has been appointed director of the Medical Neuroscience course (MedNeuro) in the Foundations Level of the Vermont Integrated Curriculum. Dr. Taylor received his M.D. from the Larner College of Medicine in 2015, joined the UVM faculty in 2020, and is currently assistant professor of neurological sciences. He completed a residency in neurology at the UVM Medical Center, followed by a fellowship in clinical neurophysiology. Dr. Taylor is the recipient of the 2015 Herbert Martin Sr., M.D. Award for Excellence in Neurology, received a 2020 Larner College of Medicine Alpha Omega Alpha Housestaff Award, and is a member of the Teaching Academy. He serves as a neurologist and co-chief of the Memory Disorders Division at the UVM Medical Center.
CITATION HIGHLIGHTS
Hernan AE, Mahoney JM, Curry W, Mawe S, Scott RC. Fine Spike Timing in Hippocampal-Prefrontal Ensembles Predicts Poor Encoding and Underlies Behavioral Performance in Healthy and Malformed Brains.Cereb Cortex. 2021 Jan 1;31(1):147-158. doi: 10.1093/cercor/bhaa216. PMID: 32860415; PMCID: PMC7727336.
Sun MM, Seleme N, Chen JJ, Zekeridou A, Sechi E, Walsh RD, Beebe JD, Sabbagh O, Mejico LJ, Gratton S, Skidd PM, Bellows DA, Falardeau J, Fraser CL, Cappelen- Smith C, Haines SR, Hassanzadeh B, Seay MD, Subramanian PS, Williams Z, Gordon LK. Neuro-Ophthalmic Complications in Patients Treated With CTLA-4 and PD-1/PD-L1 Checkpoint Blockade. J Neuroophthalmol. 2020 Oct 28. doi: 10.1097/WNO.0000000000001148. Epub ahead of print. PMID: 33136674.
Cheung KL, Tamura MK, Stapleton RD, Rabinowitz T, LaMantia MA, Gramling R. Feasibility and Acceptability of Telemedicine-Facilitated Palliative Care Consultations in Rural Dialysis Units. J Palliat Med. 2021 Jan 19. doi: 10.1089/jpm.2020.0647. Epub ahead of print. PMID: 33470899.
Edwards EM, Greenberg LT, Ehret DEY, Lorch SA, Horbar JD. Discharge Age and Weight for Very Preterm Infants: 2005-2018. Pediatrics. 2021 Feb;147(2):e2020016006. doi: 10.1542/peds.2020-016006. PMID: 33510034.
Thébaud B, Lalu M, Renesme L, van Katwyk S, Presseau J, Thavorn K, Cobey KD, Hutton B, Moher D, Soll RF, Fergusson D. Benefits and obstacles to cell therapy in neonates: The INCuBAToR (Innovative Neonatal Cellular Therapy for Bronchopulmonary Dysplasia: Accelerating Translation of Research). Stem Cells Transl Med. 2021 Feb 11. doi: 10.1002/sctm.20-0508. Epub ahead of print. PMID: 33570257.
Bruno SR, Anathy V. Lung epithelial endoplasmic reticulum and mitochondrial 3D ultrastructure: a new frontier in lung diseases. Histochem Cell Biol. 2021 Feb 18:1–10. doi: 10.1007/s00418-020-01950-1. Epub ahead of print. PMID: 33598824; PMCID: PMC7889473.
Walzl D, Solomon AJ, Stone J. Functional neurological disorder and multiple sclerosis: a systematic review of misdiagnosis and clinical overlap. J Neurol. 2021 Feb 21. doi: 10.1007/s00415-021-10436-6. Epub ahead of print. PMID: 33611631.
Short SAP, Gupta S, Brenner SK, Hayek SS, Srivastava A, Shaefi S, Singh H, Wu B, Bagchi A, Al-Samkari H, Dy R, Wilkinson K, Zakai NA, Leaf DE; STOP-COVID Investigators. D-dimer and Death in Critically Ill Patients With Coronavirus Disease 2019. Crit Care Med. 2021 Feb 12. doi: 10.1097/CCM.0000000000004917. Epub ahead of print. PMID: 33591017.
Graham SD, Tu HA, McElvany BD, Graham NR, Grinyo A, Davidson E, Doranz BJ, Diehl SA, de Silva AM, Markmann AJ. A novel antigenic site spanning domains I and III of the Zika virus envelope glycoprotein is the target of strongly neutralizing human monoclonal antibodies. J Virol. 2021 Feb 17:JVI.02423-20. voi: 10.1128/JVI.02423-20. Epub ahead of print. PMID: 33597214.
GRANTS REPORT: UVM SPONSORED PROGRAM ADMINISTRATION
Annual/Monthly Reports for Sponsored Projects
WHAT'S HAPPENING
LCOM Events Calendar | UVM Events Calendar | LCOM Student Activities Calendar
Feedback? Contact Us!
View Archive | Subscribe
Published by the Office of Medical Communications
The Larner College of Medicine
at The University of Vermont
Copyright 2021


